Manual Lymphatic Drainage: Bridging Clinical Care, Post-Surgical Recovery, and Specialist Practice
Manual Lymphatic Drainage (MLD) is no longer a niche therapy confined to specialist clinics—it has evolved significantly from its origins as a gentle therapeutic technique into a highly specialised modality with applications across clinical, post-surgical, and chronic care settings. As awareness of lymphatic health continues to grow, so too does the demand for well-trained therapists who understand both the science and sensitivity required to work within this field.
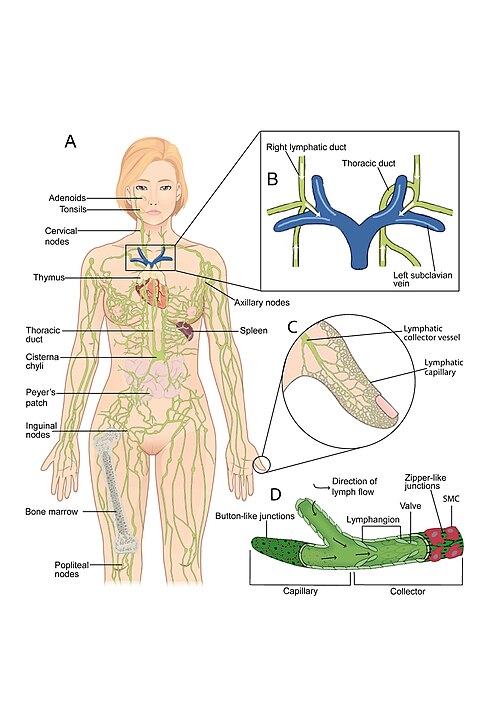
At its core, MLD is a light, rhythmical manual therapy designed to stimulate the lymphatic system, encouraging the movement of lymph fluid through vessels and nodes. Unlike traditional massage, it is not focused on muscle manipulation but on supporting a physiological system that plays a crucial role in immune function, fluid balance, and waste removal.
Understanding the Clinical Relevance of MLD
One of the most recognised applications of MLD is in the management of lymphoedema, a chronic condition characterised by swelling due to impaired lymphatic drainage. This may be classified as either primary or secondary.
Primary Lymphoedema is a congenital or hereditary condition where the lymphatic system is underdeveloped or malformed. It may present at birth, during adolescence, or later in life. MLD, when delivered appropriately, can support fluid movement, reduce discomfort, and improve quality of life, although it must be integrated into a broader management plan that may include compression and exercise.
Secondary Lymphoedema is far more common and typically develops as a result of damage to the lymphatic system. This is often seen following cancer treatments such as lymph node removal, radiotherapy, or surgical intervention. Breast cancer-related lymphoedema, for example, is one of the most prevalent forms encountered in clinical practice.
In oncology care, MLD requires a nuanced and evidence-informed approach. Therapists must understand the medical history, treatment timeline, and any contraindications or precautions.
When delivered safely, MLD can:
- Support the reduction of swelling and heaviness
- Improve tissue health and mobility
- Enhance patient comfort during recovery
However, it is essential that therapists working in this field are trained to adapt techniques for compromised systems, ensuring they do not overload or redirect fluid inappropriately.
MLD and Lipoedema: A Growing Area of Awareness
Lipoedema is a chronic and often misunderstood condition, predominantly affecting women. It involves the abnormal accumulation of adipose tissue, typically in the lower body, and is often accompanied by pain, tenderness, and easy bruising. While it is not primarily a lymphatic disorder, the lymphatic system can become compromised over time, leading to a combined presentation sometimes referred to as lipo-lymphoedema.
MLD plays a supportive role in managing lipoedema by reducing secondary fluid retention, alleviating discomfort, and improving tissue quality. It also provides a valuable therapeutic space for clients who often feel dismissed or misdiagnosed within traditional healthcare pathways. For therapists, this requires not only technical skill but also a compassionate, informed approach to care.
The Expanding Role of MLD in Post-Surgical Recovery
In recent years, the use of MLD in post-surgical care has grown rapidly, particularly within the field of cosmetic surgery. Procedures such as liposuction, abdominoplasty, breast augmentation, and Brazilian Butt Lift (BBL) all place significant stress on the lymphatic system. Swelling, bruising, fibrosis, and fluid accumulation are common post-operative concerns that can impact both recovery and final aesthetic outcomes.
MLD is increasingly recognised as a valuable intervention during the recovery phase. By encouraging lymphatic flow, it can help to reduce oedema, minimise discomfort, and support the body’s natural healing processes. Clients often report feeling lighter, less restricted, and more comfortable following treatment.
From a clinical perspective, MLD may also assist in:
- Reducing the risk of seroma formation
- Supporting the resolution of post-surgical inflammation
- Improving tissue pliability and reducing the likelihood of fibrosis
However, post-surgical MLD is not simply a wellness treatment. It requires a clear understanding of surgical procedures, healing timelines, and potential complications. Therapists must be able to recognise signs of infection, delayed healing, or adverse responses, and know when to refer to medical professionals.
Beyond cosmetic procedures, MLD is also used in recovery from medically necessary surgeries, including orthopaedic operations, vascular procedures, and cancer-related interventions. In these cases, the therapist becomes part of a wider multidisciplinary approach to rehabilitation, working alongside healthcare providers to support optimal outcomes.
The Importance of Specialist Training
As the scope of MLD continues to expand, so does the need for structured, high-quality education. Working within clinical and post-surgical environments demands more than a basic understanding of technique. It requires knowledge of anatomy and physiology at a deeper level, an understanding of pathology, and the ability to adapt treatments to complex and often vulnerable client presentations.
The Level 3 Diploma in Lymphatic Drainage: Post-Surgical, Lymphoedema and Lipoedema Care offered by Lymphaeum Education and accredited by Think Tree Hub has been designed to meet this growing demand. The course bridges the gap between holistic therapy and clinical application, equipping therapists with the skills and confidence needed to work safely and effectively in this evolving field.
Learners are guided through the structure and function of the lymphatic system, before progressing into condition-specific protocols, including lymphoedema management, lipoedema support, and post-surgical recovery techniques. Emphasis is placed on critical thinking, treatment planning, and professional boundaries, ensuring graduates are not only competent but also accountable in their practice.
Janine Wroe is the founder of Lymphaeum Education and a specialist in Manual Lymphatic Drainage (MLD), with a focus on post-surgical recovery, lymphoedema, and lipoedema care. With a background rooted in both holistic therapy and clinically informed practice, she is passionate about raising standards within the industry and bridging the gap between spa-based treatments and evidence-informed therapeutic work.
With over 20 years’ experience in adult education, Janine is dedicated to educating therapists to work safely, confidently, and ethically with complex client presentations. Through her teaching, she combines practical skill development with in-depth understanding, empowering practitioners to deliver effective, client-centred care in a rapidly growing field.
A Future-Focused Approach to Care
Manual Lymphatic Drainage sits at the intersection of wellness and healthcare. It offers a unique opportunity for therapists to support clients through some of their most physically and emotionally challenging experiences, from chronic conditions to surgical recovery.
As awareness continues to grow, so too does the responsibility of the therapist. With the right training, MLD can become a powerful tool—not just for reducing swelling, but for restoring comfort, confidence, and quality of life.
For those looking to expand their practice and step into a more specialised role within the industry, education is the foundation. The future of lymphatic therapy lies in informed, compassionate, and clinically aware practitioners who are ready to meet the needs of a changing landscape.

Janine Wroe
To find out more about the Level 3 Diploma, contact Janine at info@lymphaeumeducation.com
Contacts
Email: info@lymphaeumeducation.com